‘Ottawa’ Ottawa Hospital Looking to Renovate Intensive Care Unit for the Most Fragile Newborns
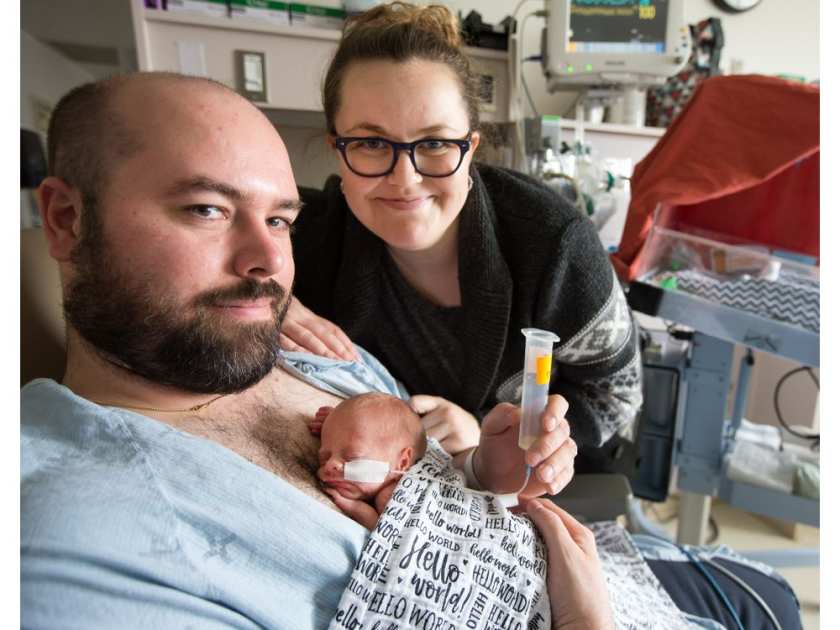
Teddy Spofford was born about two weeks ago at 30 weeks and one day gestation — almost 10 weeks before his due date.
His parents, Ryan and Victoria, spend their days travelling back and forth between their home in Kanata and the neonatal intensive care unit at the General campus of The Ottawa Hospital for five or six hours a day of providing skin-on-skin “kangaroo care” for their son, who weighed two pounds, two ounces at birth and has since climbed to two pounds, 15 ounces. Teddy spends almost all the time sleeping, just as he would if he were still in utero.
The Spoffords are pleased with the care their family is getting at the NICU. “But sometimes it feels a little crowded,” says Victoria, as the small group gathered around Teddy dodges a wheeled screen being brought into the room to offer another mother some privacy.
The Ottawa Hospital plans to renovate the NICU. It’s not just about comfort, but the long-term health of these vulnerable babies, says neonatologist Dr. JoAnn Harrold, the division head for newborn care.
Peace and quiet is crucial for babies like Teddy. The chance of survival increases with every day a baby spends in utero so that his or her organs can mature as much as possible. A baby born at 22 weeks’ gestation has a chance of survival, but it is a slim one. By 26 weeks, it’s about 90 per cent. Premature babies have immature immune, respiratory and digestive systems and may suffer from long-term health complications.
Preemies are also more likely to suffer from brain problems and need to sleep almost all of the time to help boost brain development, says Harrold. (Pregnant women often delight in their babies kicking and moving around. It doesn’t mean they’re awake — research has shown that they’re actually experiencing REM sleep.)
Improving the NICU is not just about survival, but about the best possible outcomes for babies, says Harrold. “We do an excellent job of providing for their medical needs and we’re improving all the time. But we’re working on their brain development.”
There are five neonatal care units in the city, but the 24-bed unit at the General is the largest. It is the only unit that cares for babies born at less than 30 weeks’ gestation. Patients come from all over Eastern and Northern Ontario, West Quebec and Nunavut, and about 700 babies receive care in the unit each year.
The unit at the General campus was built in the 1990s and has to adapt to new technologies as well as the needs of families. Preemies born as early as 22 weeks’ gestation currently stand a chance of surviving, something that was not possible even a few years ago, says Harrold. These babies are very fragile. They require constant vigilance and controlled temperature, humidity and an oxygen supply.
“Babies are getting smaller, but the machines that care for them are getting bigger.”
Julia Shea’s son Brady was a patient in the NICU for 68 days after he was born at 26 weeks and six days’ gestation in June 2013. He weighed two pounds, two ounces at birth.
“It was nerve-wracking,” she recalls. “There were a lot of unknowns for us. I had a fairly uncomplicated pregnancy, then my water broke at 24 weeks. Nothing can prepare you for that.”
For most of the 68 days Brady was in the unit, Shea’s daily routine meant pumping breast milk every three hours around the clock. Premature babies can’t suck on their own until about 32 weeks and are fed with a feeding tube.
Shea went to the hospital every morning at about 8 a.m and would return to her home in Kanata at about 6 p.m. For the first three days, the only contact she could have with her son was to change his diaper once a day. When her husband arrived at the unit during his lunch hour, there were often not enough chairs in the unit to go around.
“The NICU can get pretty chaotic at times with so many people coming and going, especially when doctors were doing rounds.”
Shea is now the chair of the board of directors of the Parents of Preemies Association of Ottawa (POP). Founded in 2014, the group has about 120 members. She was consulted for some of the renovation plans. Her recommendations included individual rooms for privacy, a breast pump in every room and a lounge where parents can meet each other.
“It will give us a private, peaceful place,” she says.
The renovation project, which has been approved by the Champlain Local Health Integration Network (LHIN), has now entered the “pre-capital phase,” where the hospital presents its case to the Ministry of Health and Long-Term Care. If all goes according to plan, the renovations could begin this year. The plan also calls for upgrading the existing infrastructure to improve emergency power and air handling, which will reduce the chance of infection for the babies. It will not increase the unit’s size or number of beds. The renovations will make better use of the existing site, allowing each family a little space of their own to be more involved in their baby’s care.
The changes will be done in stages to allow the NICU to continue to operate.
“The biggest thing is the space and the ability of the parent to interact with the baby,” says Harrold. “Right now, we have a limit of about two people at the bedside. We don’t even have as many chairs as there are families. This will give them the privacy to talk to their babies, or to sing a lullaby. It will allow us to customize for every patient.”
Premature baby talk
Pre-term: Any baby born more than three weeks before the expected date of birth. Human gestation is 40 weeks.
Late pre-term: Babies born at 34 to 37 weeks.
Moderately premature: Babies born between 31 and 34 weeks.
Very premature: Babies born between 27 and 30 weeks.
Micropreemie: A baby born weighing less than one pound, 12 ounces, or before 26 weeks.
Kangaroo care: A method of skin-to-skin caring for premature babies in which the baby is held by the parents for as much time as possible. This helps the baby and parents to bond, lets the baby enjoy the body warmth of a parent, and helps improve lactation for the mother.








